Медичний центр ОН Клінік
ON Clinic - міжнародна мережа медичних центрів, понад 20 з яких знаходиться в Україні. Ми використовуємо унікальний досвід лікування і сучасне обладнання. Дізнатися більше про нас

Сучасне обладнання
Всі медичні центри оснащені сучасним обладнанням, яке дозволяє точно діагностувати захворювання і проводити безопераційні процедури.

Цілодобова підтримка пацієнтів
Навіть якщо Ви зателефонуйте нам вночі в неділю, ми зможемо проконсультувати Вас, записати до лікаря або перенести дату прийому при необхідності.

Поетапна оплата
Сплачуйте частинами будь-який вид лікування. Процедура оформлення розстрочки займає всього 30 секунд, без документів і довідок про доходи.
Власна лабораторія
В усіх медичних центрах Ви можете здати аналізи. Більша частина аналізів виконується в нашій власній лабораторії «ОН Клінік».
Понад 20 медичних центрів по всій Україні
Медичний центр «ОН Клінік Харків» (м. Пушкінська). вул. Ярослава Мудрого, 30а

Медичний центр «ОН Клінік Харків» (м. Палац Спорту). пр. Героїв Харкова, 257

Медичний центр «ОН Клінік Харків» (м. Проспект Гагаріна). вул. Молочна, 48

Дитяче відділення в Харкові (м. Палац Спорту). пр. Героїв Харкова, 257

Дитяче відділення в Харкові (м. Пушкінська). вул. Я. Мудрого, 30а

YouTube ОН Клінік
Мережа медичних центрів «ОН Клінік» — якісна медицина, доступна кожному
Мережа медичних центрів «ОН Клінік» в Україні почала свою роботу у 2007 році. А сьогодні вона налічує понад 20 медичних центрів у 11 містах України.
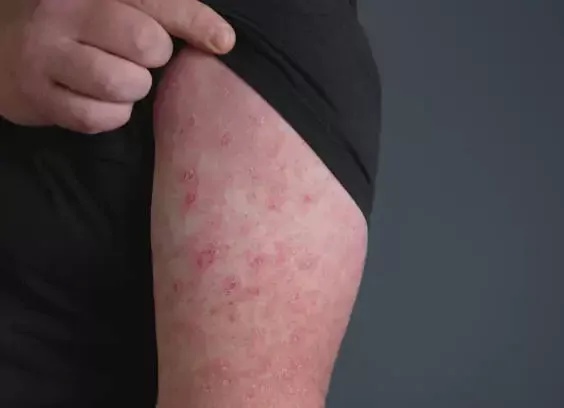
Пріоритетними напрямками Мережі є проктологія, андрологія та урологія, гінекологія, дерматологія. Наші фахівці успішно справляються з лікуванням геморою, анальних тріщин, чоловічих сексуальних розладів, захворювань жіночої репродуктивної системи, а також шкірних патологій. Однак у медцентрах здійснюють прийом пацієнтів і лікарі інших спеціалізацій.
Щоб лікування в Мережі «ОН Клінік» було комфортним для кожного пацієнта, ми:
- обладнали медичні центри за останнім словом техніки;
- підтримуємо чистоту і затишну атмосферу у всіх приміщеннях, починаючи від операційної та закінчуючи рецепшеном;
- надаємо можливість поетапної оплати лікування без документів і довідок про доходи;
- проводимо відеоконсультації для пацієнтів, які не можуть дістатися до медцентру;
- більшість досліджень біоматеріалу проводимо в нашій лабораторії;
- стежимо за якістю надання послуг, розбираючи кожне звернення відвідувачів;
- цілодобово залишаємося на зв'язку з нашими пацієнтами.
Щодня ми вдосконалюємося і працюємо над тим, щоб у стінах «ОН Клінік» кожен пацієнт не тільки отримав медичну допомогу, а й відчував себе важливим!